This is the rough narrative of a presentation on new physician literacies delivered at Stanford’s Medicine X on September 30, 2012
I’m convinced I was born at just the right time in history. I was trained as an analog physician but I’m a witness to medicine’s digital transformation. It’s really a remarkable time to be in medicine. And one of the key forces behind this transformation is information. What I’d like to talk about is how information is changing doctors and how we might begin to react.
 The paper in mama’s bag
The paper in mama’s bag
Not long ago I was treating a boy with ulcerative colitis who developed a complication of UC called sclerosing cholangitis. This is a condition where there’s autoimmune activity against the duct structures leaving the liver.
During one of his clinic visits the mother brought with her a paper that had just been published on the use of a particular antibiotic for the treatment of sclerosing cholangitis. It had been found to potentially stall the progression of the condition. The paper had been under discussion on a patient network and she wanted to know if this was an option for her son.
I looked at the paper and immediately recognized that this was in the latest edition of a journal that happened to be sitting on my desk. Mom had found the article before I had a chance to read it.
Those of you who read my blog, 33 charts, know that I’ve made a habit out of taking some of my everyday experiences and breaking them down as a means of illustrating how medicine is changing. I’d like to use this brief encounter as a jumping off point.
Breakdown | Mom beats doc
What can we learn from this?
Physicians no longer control information. While the idea of a patient bringing new research to her doctor isn’t a new phenomenon, in the broader historical context it’s huge. For the better part of civilization our role as physician has centered around privileged access to information and knowledge. But the web has created a type of disintermediation. The face-to-face encounter with a physician is evolving as a more narrowly defined element in an individual’s quest to understand their condition and get better. Access to information is the bedrock of the health 2.0 movement.
There’s too much to know. There was once a time when physicians could get their hands around what they needed to know. You’d go to the mailbox and pick up that 200 page journal and you were all set. Not so much anymore.
And honestly, a part of me felt bad. I’m a pediatric subspecialist – I’m supposed to be on top of this stuff. But had I read that that paper, there would have been another patient with with a newly released paper. There’s simply too much to know.
Information will find us. While we used to be dependent upon search in order to get the information we need, information now finds us through our social networks just as this mother did. And going forward, information will find us based on our context. The right information will find us on our smart phones depending upon where we are, what we’re doing, or what clinic we happen to be in. Social media visionary Shel Israel has suggested the last decade was about conversation, this coming decade will be about context.
We’re facing a crisis of medical knowledge
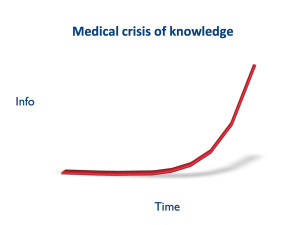
“Information is inextricably mixed with communication and sociality in a triple helix” — David Weinberger, Too Big to Know
So how have we traditionally dealt with this? In the past, medicine exerted its old-style of authority by filtering information for us. Weinberg suggests that knowledge has historically been about reducing access in order to make it more manageable.
- Medical editors decided what studies we would see.
- Librarians decided what goes on the shelf.
- Since 1910, everything doctors needed to know has always fit into 2 preclinical years.
- What patients knew was limited by what the doctor knew.
But something happened on the way to the clinic. The Internet democratized information and eliminated the traditional filters that contained medical knowledge. We suddenly were no longer limited by the space available on library shelves or the memory of a doctor.

Of course the availability of new technology to access and share information doesn’t mean that physicians will immediately begin to work and think differently. Physicians in the 21st century will need new abilities in order to function in a digital environment.
Howard Rheingold in his book Net Smart tells us that 500 years ago the appearance of the printing press didn’t immediately drive the Protestant Reformation. People first had to learn how to read.
“The interval between the technological advance of print and the social revolutions it triggered was required for literacy to spread”
So today we have the most remarkable technology emerging, but we’re creating doctors who don’t know how to read.
“We’re in a period where the cutting edge of change has moved from the technology to the literacies made possible by the technology”
So what are literacies?
Literacy was once characterized by the ability to read and write. But in modern vernacular, literacies may be viewed as the broad skill sets needed to function. Rheingold tells us, “Literacy is skill plus social competency.”
Physician literacies have traditionally been founded in an analog world. Most are centered on silo’d workflows. As doctors we needed to know how to find information in books and libraries. Handling paper medical records brought its own skill sets.
While there are many that this group could identify, I thought I would share a few critical literacies for the digital physician:
1. Network Awareness/Collaboration
Like it or not, we’re no longer alone in this, both in learning and treating. We need to learn to see ourselves as part of a broader network of collective knowledge.
2. Input management
Human attention is now the most valuable commodity and balancing information input may represent the greatest challenge of this medical generation. Clay Shirky has suggested that we’re not facing a problem of too much information, but rather filter failure.
Doctors need to understand their filters and participate in their formation. Human filtering represents one way to do that. This is how I use Twitter: I hire a few hundred people to bring me the best information available. More and more my life is about finding the right signal.
3. Creation/Translation
I’ve always wondered what it would be like if we could harness the practical knowledge and wisdom of doctors: Clinical wisdom, procedural pearls, solutions, opinions, unusual patterns, unique cases, hard-learned lessons, and even simple stories.
What if this knowledge could take the form of video, audio, images, or boluses of curated content packaged, tagged and archived so that it’s retrievable by patients and students of the next generation. That would be remarkable.
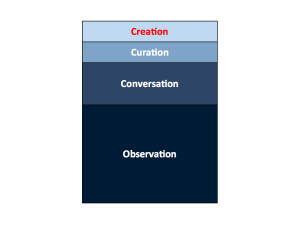
Is there a moral obligation to create? I’ve been suggesting for some time that physicians have a moral obligation to create. But I’m starting to question that. But when we look at the hierarchy of physician involvement, you see that most doctors watch, some talk, a few curate and the smallest number create. The real money in leveraging physician power may be in participation through conversation and curation. Curation can be seen as a type of literacy.
4. Mindfulness
In a world of distracting digital tools and immediately available information, we have to learn to balance technology with attention to patients. Medical mindfulness represents a new literacy that must be taught and practiced. Medical mindfulness requires intent. And despite how much information or networked knowledge exists, what matters is how we connect it to that single human encounter. What matters is that between me and that mother, we find the right information that helps both of us make the best decision. The ultimate interface is human-to-human.
This list of literacies can be discussed, adapted and built. The point is to begin a conversation.
Medicine’s culture of permission
The common denominator for many of these new literacies is involvement and contribution. Going forward, the conversion of information into knowledge can only happen in a culture of participation. Our ability to make change is dependent on our participation.
Instead we are trained in a culture of permission. Most of us believe that someone else will decide which ideas are worthy of discussion. Every idea or the creation of an idea is something that needs some kind of validation. We’re a profession of information isolation.
Information is extending who we are
Machines have already extended and even replaced what we can do with our hands, our eyes and our ears. Intelligent networks will extend what we do with our minds. Information and how it’s accessed represents an example of our entrée into a new era of posthuman medicine. We need to begin to think about where we fit into the bigger picture of a knowledge network.
I have to finish with this quote from media visionary, Marshall McLuhan. What’s more remarkable than the fact that he so clearly envisioned the internet is the fact that he did it in the early 60’s.
In this electric age we see ourselves being translated more and more into the form of information, moving toward the technological extension of consciousness. — Marshall McLuhan, Understanding Media, 1964
Information will redefine us. The way we view it, hear about it, access it, store and organize it. How we react to it as a profession will determine where we go.
Links to Amazon represent affiliate links.
